The Lancet Launches Important New Guidance On Dementia Risk Reduction
The Lancet has launched new guidance which reveals that an extended set of 12 modifiable risk factors might prevent or delay up to 40 per cent of dementia cases globally.
The report ‘Dementia prevention, intervention, and care: 2020 report of the Lancet Commission’ updates on previous evidence from the 2017 Lancet Commission on dementia prevention, intervention, and care, and was launched today during a live session of the Alzheimer’s Association International Conference (AAIC 2020).
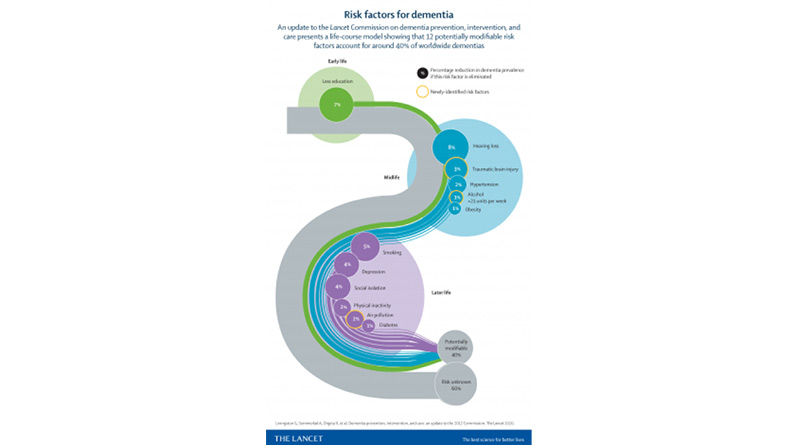
A key finding of the report is the addition of three new dementia risk factors: excessive alcohol consumption, head injury and air pollution. These build on the nine already-established risk factors set out in the 2017 report: less education, hypertension, hearing impairment, smoking, obesity, depression, physical inactivity, diabetes, infrequent social contact. Together, modifying these risk factors at the population level could potentially prevent or delay up to 40 per cent of dementia. Interestingly, the potential for prevention is high and might be higher in low-income and middle-income countries (LMIC) where the prevalence of dementia is higher, and where access to information and education around dementia risks is often more limited.
The report’s lead author, Professor Gill Livingston of University College London, speaking from London, said: “Our report shows that it is within the power of policy-makers and individuals to prevent and delay a significant proportion of dementia, with opportunities to make an impact at each stage of a person’s life. Interventions are likely to have the biggest impact on those who are disproportionately affected by dementia risk factors, like those in low- and middle-income countries and vulnerable populations…”
The report’s findings have implications for individuals and importantly for governments to implement interventions to reduce dementia – especially the factors of less education and air pollution but governmental interventions and public health messaging are equally required for the individual risk factors and world governments must look at all stages of life when formulating their dementia risk reduction policies.
Hearing loss is an example where a joint responsibility approach between individual and government is required. The recommendation around hearing loss, for instance, that individuals should use hearing aids, must be accompanied by a recognition that hearing impairment can cause social disconnection; a characteristic often shared following a dementia diagnosis. Policy makers have a responsibility to provide risk reduction information and awareness around hearing loss and post-diagnostic psychosocial support to those diagnosed with dementia – and also carers – to ensure they continue their social activities.
ADI’s Chief Executive Paola Barbarino, said: “Delving into the report is really worth it as there are many more gems to discover, for example education is really important until 20 years of age, after that learning may not be such a key factor. An emphasis on promoting educational development at a young age has never seemed so crucial. Early retirement, which is perceived by many as a desirable outcome, may actually increase our chances to develop the disease. I know how hard it is to persuade those with hearing loss to wear hearing aids but there has never been a more compelling case to start using them as they are a protective factor.
Many of the great suggestions in the report can also help reduce the risk factors of other important diseases and conditions – diabetes, heart disease and cancer for example – and I hope this will inspire more people to make lifestyle changes. The fact that many of these lifestyle changes can be effective even if started later in life should also be a further motivation to get going as soon as possible.
Overall the fact that so many studies are happening at the same time is cause of joy and elation. Yes there is a lot still to do – there remain 60% of unknown risks factors – but also so much that has been done and these findings need to be distilled and brought to a larger audience. The beauty of this report is that it focuses on both population-wide recommendations for policy makers and governments and tangible action that individuals can take to reduce their risk. It recognises gaps in data and encourages further research into low- and middle-income countries and calls for more resources to support people living with dementia and their families as well as addressing inequalities. All of these could be achieved if every nation adopted the WHO’s Global action plan on the public health response to dementia and we will continue to promote this at all levels in the next few years.
The report quotes ADI’s figures: the global prevalence of dementia is over 50 million and will rise to 152 million by 2050, and the annual global cost of dementia is US$1 trillion.
The COVID-19 pandemic has and will continue to present additional challenges for individuals living with non-communicable diseases (NCDs), who are predisposed to more severe symptoms of coronavirus and to developing additional co-morbidities. For example, the evidence on the preventative effects of sustaining physical exercise in midlife (and possibly later life) on dementia is strongly linked to decreasing the risks associated with obesity, diabetes, and cardiovascular disease.
The recommendation of keeping cognitively, physically, and socially active in midlife and later life here becomes especially poignant in the context of social distancing measures. Each government must therefore take into account NCD and dementia risk factors in their COVID-19 responses plans.
