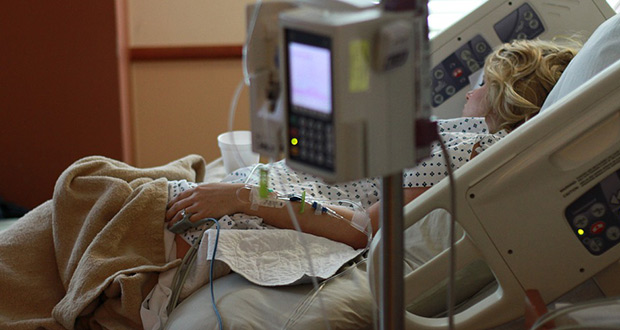
Nine Out Of 10 Nurses Have Witnessed Dying Patients Stranded In Hospital
 Nine out of 10 (94%) UK nurses say they have seen dying patients stranded in hospital as a result of delays in funding that would have otherwise allowed them to be cared for at home or in the community. Six out of 10 (62%) say it is a common occurrence and more than half (54%) think that the number of patients stuck in hospital has increased since last year.
Nine out of 10 (94%) UK nurses say they have seen dying patients stranded in hospital as a result of delays in funding that would have otherwise allowed them to be cared for at home or in the community. Six out of 10 (62%) say it is a common occurrence and more than half (54%) think that the number of patients stuck in hospital has increased since last year.
An acute trust nurse responding to the survey commented: “Fast track services to get patients home where they want to die [are] not very fast. Patients often die with us in hospital before they’re able to get home.”
Nurses were also worried about the impact of this year’s winter pressures on end of life care. Almost eight out 10 (77%) feel they have had a negative effect on the quality of care they are able to provide to dying patients and 43% think the impact has been worse than last year.
A surgical ward staff nurse responding to the survey commented: “Patients wait on trolleys in A&E for hours, even days due to bed shortages, only to be transferred to a ward with staff shortages. It is difficult to provide a high level of care when you are trying to focus on so many things at once. It should be a privilege to nurse a person in their final days of life. Sometime we might be the only people they have.”
Many also raised concerns that patients are dying alone in hospitals and in the community because there are too few staff to spend time with them. Others had seen patients die in emergency departments while waiting for transfers to wards or hospices.
A nurse responding to the survey commented: “I have unfortunately experienced patients without families dying alone in rooms due to staff shortages. I am often unable to attend to families right away following the death of a loved one due to needing to administer medications.”
The survey of more than 600 nurses, by Nursing Standard and Marie Curie, highlights how end of life care is being compromised by pressures on the NHS. The survey has also found that:
- Almost two-thirds (65%) of nurses say they do not have sufficient time to provide high quality care for patients who are dying, a similar proportion to those who answered the survey last year.
- Staffing levels (38%) and time constraints (25%) were the main barriers identified to providing high quality care, followed by a lack of care provision in the community, including care homes, peoples’ homes and hospices.
Anne Cleary, Deputy Director of Nursing for Marie Curie, said: “The results illustrate the unsustainable pressure being placed on nurses while they shoulder the huge responsibility of caring for people at the end of their lives. Nurses go to work each day because they want to provide high quality care. Not being able to meet those standards, can then put real pressure on how they feel about their job, not to mention the unnecessary pain and distress it causes for patients and their loved ones.
“Nurses have told us that they are caring for more and more people who are dying in hospital when don’t need to be there. Now, more than ever, we need to support them by investing in community care so that people can get the nursing they need at the end of their lives outside of hospitals, in a place of their choosing.
Graham Scott, Editor of Nursing Standard, said: “These survey results highlight how the time and staffing pressures facing nurses are having a worrying impact on their ability to care for patients in their final days of life.
“Funding delays are also preventing dying patients from leaving hospitals to spend the end of their life at home with their loved-ones or being cared for within the community. Nurses must have the resources they need to see patients have the very best care at what is an extremely difficult time for them and their families.”
Eleanor Sherwen, the RCN’s professional lead for end of life and palliative care, said: “The results of the survey are disappointing but not surprising. We only have one chance to get end of life care right. How people die remains in the memories of their loved ones for a long time. Nurses are doing their best in incredibly challenging circumstances but there is a lack of time.
“We need training and education for nurses, action on nursing recruitment and retention, particularly in district nursing workforce, and a social care workforce who can support district nurses. Health and social services need to work together.”
The full results of the survey are available here www.rcni.com/marie-curie-findings.

